general reconstruction instructions
Skin graft
Positioning
After skin grafting, it is very important to protect the area where the graft was placed. If the skin graft was applied to the leg, it is of upmost importance to keep the leg elevated with your knee straight. If you are sitting in a chair, keep the affected leg elevated on a pillow on an adjacent chair. Don't sit with the leg down, because this can jeopardize the success of the graft for the first couple weeks after surgery.
Activity
Dr. Gimbel requests that you do not walk on a grafted leg for two weeks after surgery if the graft is at or below the knee, as this can jeopardize the success of the graft. Otherwise, care should be taken to avoid putting pressure on the graft site.
Dressings
Donor Site:
Keep the xeroform (yellow gauze) on the donor site (where the graft came from) and leave it open to air to dry out. After it is dry, it is OK to shower over it (if Dr. Gimbel has given the OK for showers). Just let it dry out again for 30-60 minutes after the shower so it doesn't stick to your clothes. There is no need to place additional dressings on the donor site, as these will just stick and make removal more painful.
Recipient Site:
The skin graft recipient site (where the graft was placed) is delicate. Please try to protect it from pressure, shearing, and trauma. Dressing changes are generally done every other day with xeroform (yellow gauze), followed by dry 4x4 gauze and/or ABD pad, followed by ACE wrap (if on the extremity). Your visiting nurse can do these dressing changes, but so can a friend or family member (once educated). When peeling off the xeroform from the graft site, pretend it is like opening a sardine can. Pull the xeroform backwards along the skin instead of up and away from the skin. Thuis methods lessens the chance of the graft getting pulled up with the dressing.
Do not wash, scrub or rinse the graft site for 2 weeks after surgery. Usually, Dr. Gimbel will give you the OK to wash when he sees you in clinic. If he has not given you the OK, don't wash.
Once Dr. Gimbel has removed all of the xeroform from both the donor and recipient sites (about three weeks), it is good to gently apply Vaseline Intensive Care lotion to each site twice a day to prevent scaling and cracking. You should continue to apply lotion to these sites for months, as the skin is remodeling.
After skin grafting, it is very important to protect the area where the graft was placed. If the skin graft was applied to the leg, it is of upmost importance to keep the leg elevated with your knee straight. If you are sitting in a chair, keep the affected leg elevated on a pillow on an adjacent chair. Don't sit with the leg down, because this can jeopardize the success of the graft for the first couple weeks after surgery.
Activity
Dr. Gimbel requests that you do not walk on a grafted leg for two weeks after surgery if the graft is at or below the knee, as this can jeopardize the success of the graft. Otherwise, care should be taken to avoid putting pressure on the graft site.
Dressings
Donor Site:
Keep the xeroform (yellow gauze) on the donor site (where the graft came from) and leave it open to air to dry out. After it is dry, it is OK to shower over it (if Dr. Gimbel has given the OK for showers). Just let it dry out again for 30-60 minutes after the shower so it doesn't stick to your clothes. There is no need to place additional dressings on the donor site, as these will just stick and make removal more painful.
Recipient Site:
The skin graft recipient site (where the graft was placed) is delicate. Please try to protect it from pressure, shearing, and trauma. Dressing changes are generally done every other day with xeroform (yellow gauze), followed by dry 4x4 gauze and/or ABD pad, followed by ACE wrap (if on the extremity). Your visiting nurse can do these dressing changes, but so can a friend or family member (once educated). When peeling off the xeroform from the graft site, pretend it is like opening a sardine can. Pull the xeroform backwards along the skin instead of up and away from the skin. Thuis methods lessens the chance of the graft getting pulled up with the dressing.
Do not wash, scrub or rinse the graft site for 2 weeks after surgery. Usually, Dr. Gimbel will give you the OK to wash when he sees you in clinic. If he has not given you the OK, don't wash.
Once Dr. Gimbel has removed all of the xeroform from both the donor and recipient sites (about three weeks), it is good to gently apply Vaseline Intensive Care lotion to each site twice a day to prevent scaling and cracking. You should continue to apply lotion to these sites for months, as the skin is remodeling.
Leg and foot reconstruction
other reconstruction
Drain care
|
What is a JP drain?
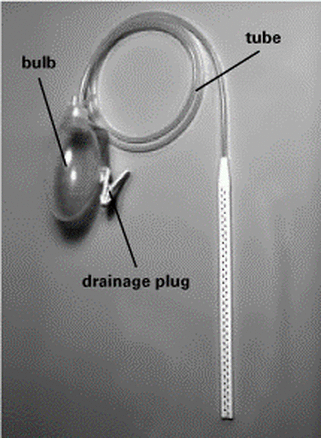
A Jackson-Pratt (JP) drain is a type of drain that is placed in an incision during surgery. The drain is made up of a hollow tube that is connected to an egg-shaped bulb. The hollow tube begins inside the incision and exits the body. Attached to the end of the tube outside of the body is the collection bulb. This bulb collects fluid from the incision (see diagram below). What does a JP drain do? The JP drain helps drain excess blood and fluid from under the skin and the incision site. When you squeeze the egg-shaped bulb, fluid is sucked out. If the bulb is not squeezed tightly, the fluid will not drain. Why is the JP drain needed? The JP drain helps to keep fluid from collecting in the wound. It does this by removing the excess blood and fluid from under the skin and in the incision. The JP drain is temporary. It stays in place until the drainage has slowed down or stopped. As healing occurs, the fluid collected in the drain bulb should change color. It becomes less bloody, and the amount gradually decreases. Your doctor will decide when the drain should be removed. It will be removed in your doctor’s office. How do I care for the JP drain at home? Pin your JP drain to your clothing by using a safety pin through the plastic loop on the top of the bulb. If the drain is not attached to your clothing, it may pull out from under your skin. Also, a drain usually feels more comfortable when it is attached. To care for the JP drain at home, you will have to empty the drain and change the dressing. Emptying the drain You will need: --the measuring cup provided by the hospital, or a similar small measuring cup used exclusively for this purpose. --paper to make a daily JP drainage chart for each drain. Record AM drainage and PM drainage each day and record. 1. Wash your hands with soap and water. 2. Hold the drain securely. 3. Remove the drainage plug from the emptying port. 4. Carefully turn the bulb upside down over the measuring cup, and gently squeeze all of the drainage into the measuring cup. 5. Squeeze the middle of the bulb. 6. While still squeezing the bulb, replace the drainage plug. This step is important to keep the drain sucking. 7. Measure how much fluid you removed from the bulb. 8. Write down the amount of the fluid you removed from the bulb. If you have more than one drain, keep a separate record for each one. 9. Empty the fluid into the toilet and flush. 9. Rinse the measuring cup, and wash your hands with soap and water. 10. You should empty the drain at least two times each day, in the morning and at bedtime. Stripping the Drain To prevent clots from blocking the drain, you will need to “strip” it. Stripping means that you use your fingers to squeeze along the length of the drain to help maintain the flow of drainage. 1. Using one hand, firmly hold the tubing near the insertion site (close to your skin). This will prevent the drain from being pulled out while you are stripping it. 2. Using your index finger and thumb of the other hand, squeeze the tubing below the first hand. You should squeeze it firmly enough so the tubing becomes flat. 3. As you are squeezing, slide your index finger and thumb down the tube about 6 inches toward the bulb. Then, release the tubing held by the hand closest to your body. Repeat. 4. Do not release the pressure you are creating in the tubing until you reach the bulb. 5. Strip the drain each time you empty it. |